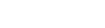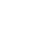Healthcare contract management software is a platform for managing the full lifecycle of every agreement a healthcare organization handles, from physician employment contracts and payer agreements to BAAs, vendor deals, equipment leases, and research partnerships.
That definition is not wrong, but it's incomplete. Because the thing nobody tells you about healthcare contract management is that the hard part isn’t HIPAA. Every serious platform is HIPAA compliant.
The hard part is that a single hospital generates nine fundamentally different types of contracts, each with different owners, different timelines, and different compliance traps.
And they all need to live somewhere findable.
TL;DR
- Healthcare’s real contract management problem isn’t compliance. It’s variety. Nine contract types, different schedules, different departments, one building.
- Every vendor leads with HIPAA. But HIPAA-first buying pushes hospitals toward rigid enterprise tools, and that’s how contracts end up scattered across three systems with nobody tracking renewals.
- IBM’s 2025 data: healthcare breaches still cost more than any other industry at $7.42 million per incident. Contract documentation gaps are what turn breaches into six-figure settlements.
- Most “healthcare CLM” platforms are enterprise tools with a healthcare landing page. What hospitals actually need is flexibility across nine contract types in one affordable, searchable platform.
- ContractSafe: HIPAA and SOC 2 compliant, unlimited users, AI extraction, live in under 30 minutes.
What Nine Types of Contracts Actually Look Like at a Healthcare Org
It’s 10 AM at a mid-sized hospital. In radiology, the director just got a reminder that the imaging system lease renews in 90 days. The MRI vendor wants a 12% price increase and a five-year commitment.
She needs the current lease terms, the maintenance history, and the original equipment evaluation, and she needs them before her meeting at 2 PM.
Down in HR, someone is onboarding a locum tenens cardiologist for a six-week coverage gap. The staffing contract needs credentialing verification, malpractice tail coverage, and specific on-call terms.
HR wants to use the last locum tenens agreement as a starting template. Nobody knows which shared drive it’s on.
Finance is renegotiating reimbursement rates with three payers simultaneously. Each contract has different covered services, different payment timelines, and different dispute resolution terms. The CFO wants a side-by-side comparison. Finance has the contracts in three different folders.
Meanwhile, compliance just discovered that a billing vendor who’s been handling patient data for two years never signed a BAA. Nobody flagged it because the vendor was onboarded during a staffing transition.
The original point of contact left the organization eight months ago.
And the OR director needs an amendment to an equipment maintenance agreement, because the surgical robot’s service terms changed when the manufacturer got acquired last quarter.
All of this is happening in the same building, on the same Wednesday, and nobody has a single view across all of it.
That’s nine categories of healthcare contracts in practice. Not as a list of definitions, but as simultaneous operational problems hitting different departments on different schedules.
According to AHRMM, the average hospital manages over 1,200 GPO and local contracts and activates pricing for more than 40,000 new line items every six months. That’s the supply chain alone.
Add physician agreements, payer contracts, BAAs, technology licenses, and staffing deals, and the total contract portfolio for a mid-sized hospital is enormous.

What Goes Wrong When Nobody Can See Across All of It
In June 2019, a phishing campaign hit PIH Health, a healthcare system in Southern California. Attackers compromised 45 employee email accounts. The protected health information of 189,763 individuals was exposed.
The Office for Civil Rights investigated. What they found wasn’t just a cybersecurity failure. PIH Health’s risk analysis was inaccurate. Security measures were insufficient. Audit review processes were weak. PIH Health paid $600,000 to settle.
Every vendor with access to those email systems should have had a BAA specifying security requirements, breach notification timelines, and audit rights.
The “inaccurate risk analysis” finding suggests PIH Health couldn’t demonstrate what their contracts required of their vendors. That’s not a security problem. That’s a contract visibility problem.
This is the pattern OCR sees over and over. The breach gets the headline. The investigation uncovers contract gaps underneath: missing BAAs, outdated security language, no documentation of vendor compliance reviews.
IBM’s 2025 Cost of a Data Breach Report found that healthcare data breaches still cost more than any other industry, averaging $7.42 million per incident. Healthcare has held the top spot for 14 consecutive years.
The breach lifecycle in healthcare averages 279 days, five weeks longer than the global average.
The breach gets the fine. The contract gaps are what made the fine possible.
Why HIPAA Compliance Is Table Stakes for Healthcare Contract Management
Go shopping for healthcare contract management software and you’ll notice something. Every vendor leads with HIPAA. HIPAA compliance. HIPAA-ready. HIPAA built in. It’s on every homepage, every feature page, every comparison chart.
Which makes sense. HIPAA compliance is mandatory. But it’s also table stakes. Listing it as a differentiator is like a restaurant advertising that they wash their hands. You’d be alarmed if they didn’t.
The problem with the HIPAA-first framing is what it does to the buying decision. It trains healthcare buyers to evaluate CLM platforms on compliance checkboxes.
That leads them toward expensive, rigid, healthcare-specific enterprise tools that do one thing well (compliance documentation) but can’t flex across nine contract types without a six-figure implementation.
The real risk for most hospitals isn’t failing a HIPAA audit. It’s having contracts scattered across three systems because no single platform could handle all of them.
The radiology lease is in one tool. The payer contracts are in a spreadsheet. The BAAs are in a shared drive. And the staffing agreements are in someone’s email.
That fragmentation is where missed renewals, unsigned BAAs, and expired terms actually live. Not in a compliance checkbox gap.
What Flexibility Actually Means in Practice
Go back to that morning at a hospital. Same building, same problems, different outcome.
-
Radiology: The director opens one platform and searches for the imaging system lease by vendor name. Current terms, maintenance addendum, original evaluation, all linked. The renewal alert already went out 90 days ago to her and the CFO.
-
HR: Searches “locum tenens cardiologist.” Finds the last staffing agreement. The AI already extracted the key terms: compensation structure, coverage dates, malpractice requirements. They use it as a starting point.
-
Finance: Pulls up all three payer contracts with a filtered search. Same platform, same format, side by side.
-
Compliance: Runs a query for every vendor relationship without a signed BAA. The platform flags the billing vendor in about four seconds.
-
OR: Finds the equipment maintenance agreement, sees the amendment history, knows who last modified it.
Same building. Same Wednesday. Same nine contract types. One platform that’s flexible enough to handle all of them, not because it was built exclusively for healthcare, but because it was built to handle any contract type well.
That’s what ContractSafe does. It’s HIPAA and SOC 2 compliant (check the box).
But the real value is that it handles physician agreements, payer contracts, BAAs, equipment leases, vendor deals, staffing agreements, and technology licenses in one searchable place with role-based permissions that let every department access what they need.
The Enterprise Healthcare CLM Tax
Most platforms marketed as “healthcare contract management software” are enterprise CLM tools with a healthcare landing page. They come with per-seat pricing, six-month implementations, and feature sets designed for legal departments at Fortune 500 companies.
That’s fine if you’re a 30-hospital system with a dedicated legal ops team. But most healthcare organizations aren’t that. They’re a 200-bed community hospital where the person managing contracts is also managing three other things.
Per-seat pricing is especially brutal in healthcare. Think about who needs contract access at a single facility:
- The radiology director
- The OR manager
- The HR coordinator
- The compliance officer
- The CFO
- The payer relations team
Multiply that across departments, and per-seat licensing adds up fast.
ContractSafe takes a different approach: unlimited users on every plan, with pricing based on contract volume instead of headcount.
With HIPAA Security Rule changes expected to be finalized in 2026 that would require annual compliance audits and mandatory safeguards, the urgency to get organized is real.
But a six-month implementation doesn’t help when the deadline is this year. ContractSafe has most teams live in under 30 minutes. No consultants. No IT project. Just contracts, searchable, from day one.
How ContractSafe Makes Healthcare Contract Management Easier
ContractSafe is the CLM software built for teams who want power without the pain. You get everything you need to manage contracts from intake to execution to renewal, with no steep learning curve.
Most teams are live in under 30 minutes. The AI extracts key terms and identifies execution status automatically. You get enterprise-grade security (SOC 2, HIPAA, full audit trails) with everything searchable in one place.
Support comes from real humans on every plan. Custom dashboards and reports come standard.
If you’ve been burned by overbuilt CLM platforms in the past, this one’s for you.