Every hospital has a pharmacy. And in that pharmacy, every medication is tracked — dose by dose, interaction by interaction, expiration date by expiration date.
Miss one refill and a patient's treatment plan falls apart. Mix up one dosage and you're looking at a malpractice claim.
Your contracts deserve the same discipline. But they almost never get it.
And the regulatory environment isn't getting simpler. HIPAA Security Rule changes expected to be finalized in mid-2026 would make all safeguards mandatory — no more "addressable" loopholes.
They'd also require annual compliance audits and impose 24-hour breach reporting on business associates. If your contracts aren't locked down, your compliance posture isn't either.
So whether you're building a new contract from scratch or auditing one that's been gathering dust since 2019, this guide walks through the nine types of healthcare contracts you need to know — plus practical advice on how to actually manage them.
For a deeper dive into the big picture, check out our full guide on contract management in healthcare.
TL;DR
-
Major HIPAA Security Rule changes are expected in 2026, making audit-readiness more urgent than ever.
-
There are nine common types of contracts used in the healthcare industry. Plus two “honorable mentions” to watch: supply chain/vendor and managed care/payor agreements.
-
Every contract type comes with its own compliance traps — Stark Law, Anti-Kickback Statute, HIPAA/BAA requirements, and EMTALA provisions can all apply depending on the agreement.
-
While your facility might not use all nine, it’s super important to know which ones to use, when to use them, and how to execute each one properly. Build in Stark/AKS, HIPAA/BAA, and EMTALA checks where appropriate, and review compensation for fair market value annually.
-
That’s only part of it. The rest? Staying hyper-organized and creating a process for managing contracts at your healthcare business. Modern CLM software with AI (alerts, clause/term extraction, OCR search) reduces risk and speeds audits.
-
Healthcare contract management software like ContractSafe turns the chaos into something searchable, trackable, and audit-ready.
9 Most Common Types of Healthcare Contracts
1. Physician Recruitment Contract
A physician recruitment contract spells out the strategies and incentives used to attract physicians to your facility. Relocation assistance, student loan forgiveness, signing bonuses — the works.
Getting this one right matters more than most people realize. Your facility has to comply with Stark Law and the Anti-Kickback Statute, which means every incentive needs to be carefully structured.
If you accept Medicare or Medicaid (and who doesn't), the scrutiny is even tighter.
The key compliance move: document that all support is tied to genuine community need — not to referral volume. Link every compensation term to fair market value. And review that valuation annually, not just when the contract is signed.
Compliance tip: Document relocation/loan forgiveness terms, link support to community need (not referrals), and confirm all compensation aligns with fair market value.
2. Physician Employment Contract
A physician employment contract defines the full relationship between a physician and your facility. Schedule expectations, compensation structure, benefits, on-call requirements — all the standard stuff.
But the details that matter most are the ones people skim past. Termination clauses (for-cause and without-cause), malpractice coverage type (claims-made versus occurrence), who pays for tail insurance, and dispute resolution mechanisms.
These are the provisions that come back to haunt you when a relationship ends badly.
Most physician employment contracts also include a restrictive covenant — healthcare's version of a non-compete. But here's a heads-up: enforceability varies wildly by state, and federal scrutiny has intensified.
Several states now restrict physician non-competes altogether. Talk to counsel before including one, and definitely before trying to enforce one.
Also good to know: Most physician employment contracts include a restrictive covenant, which is fancy healthcare speak for a “non-compete.” This covenant addresses requirements related to the physician competing with the facility post-employment, placing restrictions on soliciting patients, or working for another facility in the same geographic area.
Note: Non-compete enforceability varies by state, and federal rulemaking has increased scrutiny; several states restrict physician non-competes. Consult counsel before including or enforcing.
3. Medical Director Contract
A medical director agreement outlines what a physician does in an administrative leadership role — compensation, term length, termination procedures, specific responsibilities including admin tasks and on-call hours, malpractice and liability coverage, and non-compete/non-solicitation clauses.
AKS/Stark alert: compensation must reflect documented administrative services that are actually performed. Not referrals. Not patient volume. Actual services. And that compensation needs to align with fair market value, reviewed on a regular basis.
In 2024, Community Health Network settled with the DOJ for $345 million over Stark Law violations tied to physician compensation arrangements. It was the largest such settlement ever. The takeaway isn't subtle.
4. Patient Transfer Contract
When a patient's care is transferred from one physician or facility to another, you need a patient transfer contract. These typically cover care duration, termination conditions, each party's responsibilities, billing details, and insurance information.
EMTALA is the big one here. Your contract needs to define clinical criteria for transfer, stabilization requirements, documentation protocols, and who's responsible for transport.
Liability allocation and communication protocols between the sending and receiving facilities should be spelled out clearly enough that a 2 AM handoff goes smoothly.
5. Equipment Lease Contract
Healthcare equipment is absurdly expensive, which is why most facilities lease rather than buy. The equipment provider usually supplies the lease contract, but knowing what to look for keeps you from getting stuck with bad terms.
Standard provisions include equipment description, lease duration, fee schedule, consequences for missed payments, and return conditions. A good contract also covers damage and repair responsibilities.
But in healthcare, there's a layer most lease templates miss: any device that stores PHI needs data handling and sanitization provisions.
You also want maintenance and calibration obligations, uptime SLAs, and upgrade or refresh options. Medical technology evolves fast. Your lease terms should account for that.
6. Managed Services Contract
Coding, transcription, billing collections — healthcare businesses outsource a lot of operational functions. If your facility is one of them, a managed services contract is non-negotiable.
These agreements cover scope of work, timelines, cost schedules, payment terms, and termination procedures. But for healthcare, you need to go further.
Add service-level agreements with measurable KPIs, cybersecurity and incident response requirements, HIPAA Business Associate Agreements for any vendor handling PHI, audit rights, and clear exit/transition assistance if you need to switch providers.
That last point — transition assistance — is the one everybody forgets until they're trying to leave a vendor and realize their data is effectively held hostage. Write the exit into the entrance.
7. Purchased Services Contract
If your facility works with third-party non-employee contractors (take a second read on that phrase if you need to — it's a mouthful), a purchased services agreement is probably in order.
These cover everything from environmental services and laundry to maintenance and specialized clinical support.
Why it matters: Purchased services can account for roughly 30–35% of a hospital’s operating expenses; routine audits and benchmarking uncover savings. Include deliverables, pricing protections, quality standards, and termination for convenience.
And those costs are climbing — purchased service expenses rose 9.5% year-over-year as of early 2025, according to Kaufman Hall data. Routine audits and benchmarking of these contracts can uncover real savings.
Include clear deliverables, pricing protections, quality standards, and termination for convenience. And actually audit them. Regularly.

8. Technology Licensing Contract
Healthcare facilities rely on advanced technology, and most of it requires a licensing agreement. The good news: the technology vendor typically creates and provides the contract. The bad news: that means the terms are written in their favor.
Standard provisions include what technology is covered, how your facility can use it, contract duration, licensing fees, prohibited activities, and termination conditions.
For healthcare, add BAAs when vendors access PHI, specified user limits, data ownership and portability clauses, breach notification timelines, and de-identification/data use agreements if the vendor wants to use your data for analytics or research.
With AI tools increasingly touching clinical workflows and patient data, these provisions matter more every year.
9. Joint Venture Contract
When your organization partners with another entity on a shared project — a new outpatient clinic, a research initiative, a specialized service line — you need a joint venture contract.
These agreements define each party's financial responsibilities, their activities and involvement, and how risks and rewards are shared. The governance details are critical: board composition, reserved matters, capital call provisions, the regulatory compliance plan, non-compete/non-solicitation clauses, and exit or buy-sell mechanics.
Joint ventures in healthcare also need to account for the regulatory complexity of both parties. A compliance plan that covers one partner but ignores the other isn't a compliance plan at all.
Other Common Agreements to Track (Beyond The 9 Above):
-
Supply chain and vendor agreements: contracts with distributors, group purchasing organizations (GPOs), and consumable suppliers. These should include quantity commitments, pricing protections, and delivery SLAs.
-
Managed care and payor agreements: HMO, PPO, and ACO contracts that define reimbursement schedules, utilization management terms, and value-based care benchmarks. As the industry continues shifting toward value-based models, these agreements are becoming more complex and more consequential.
How to Manage Healthcare Contracts: 3 Things to Keep in Mind
You know your contracts. You know the types. Now for the part that actually determines whether all of this works in practice: management.
Here are three things every contract manager in healthcare should be thinking about.
1. Your Contracts Must Be Customized
Templates are great for getting started. They're terrible as finished products.
Every healthcare contract needs to be customized to the specific agreement it governs. The details that make a contract protective — and enforceable — are the ones specific to your relationship with the other party.
Build checklists for healthcare-specific clauses: BAAs, EMTALA transfer criteria, Stark/AKS attestations, fair market value documentation, and value-based care metrics like readmission rates or care coordination benchmarks. Standardize clause libraries and playbooks so the right language surfaces every time.
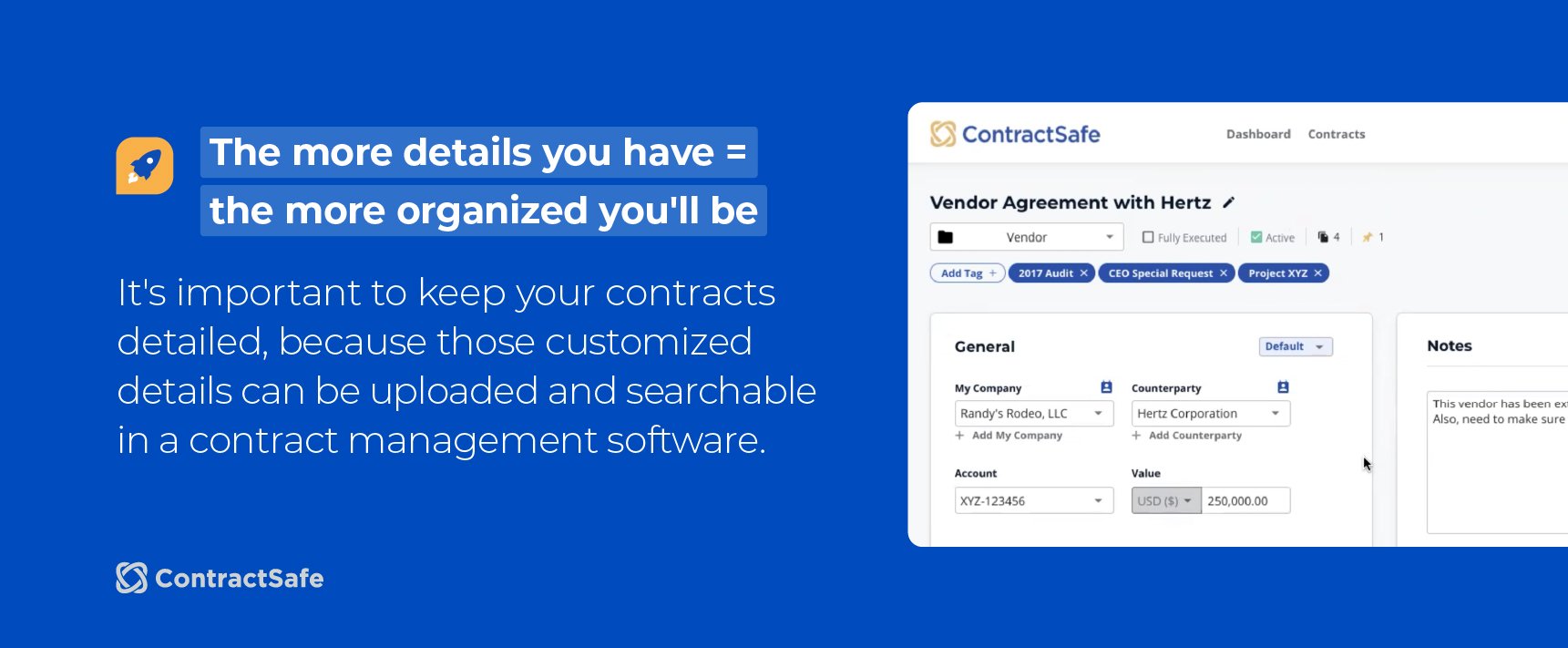
Here's the organizational payoff: when your contracts are detailed, those customized details become searchable data in a contract management system. The more specific you are up front, the easier everything is to find later.
2. You Need a Contract Review Process
Signing a contract isn't the finish line. It's the starting line.
After execution, you need a review process to confirm the contract is valid, complete, and properly stored. Multiple people should review each contract to ensure both parties have signed and fulfilled their obligations correctly.
This is also when you log every critical date — renewals, expirations, insurance certificate deadlines, price escalators, performance review milestones. Enter all of it into a management system so you don't accidentally let a contract lapse or auto-renew on unfavorable terms.
Set automated alerts for all of it. Then set annual compliance checks to confirm fair market value and regulatory alignment.
With HIPAA Security Rule changes potentially requiring annual audits by late 2026, getting this process buttoned up now is more than good practice — it's preparation.

3. You Need a Way to Store Your Contracts
This sounds basic. It's not.
Secure storage isn't just about having a folder somewhere. It means role-based permissions, audit logs, encryption, and accessibility controls that protect contracts from both external threats and internal mishandling.
Unless your facility plans to keep doing things the old way (and honestly, the old way is a liability at this point), healthcare contract management software is worth the investment.
The right platform stores, organizes, and secures your contracts while giving you OCR search across scanned documents, AI-powered clause and term extraction, e-signature integrations, and configurable workflows.

A platform like ContractSafe also eliminates the need for rigid file naming conventions. When you can tag by counterparty, contract type, date, and custom fields, you can search and run reports with a click.
No more guessing whether the file is called "VendorAgreement_FINAL_v3" or "VA_signed_052024."
Bulk imports with AI field mapping also cut onboarding time dramatically. And dashboards help you spot at-risk contracts before they become at-risk situations.